It’s also possible that some drugs that are used to treat COVID-19 in people who are seriously ill, may contribute to kidney damage. Low oxygen levels can cause many organs and tissues, including the kidneys, to not function properly. low oxygen: Pneumonia due to COVID-19 can mean that less oxygen is entering your blood than usual.This can block blood flow and lead to kidney damage. These clots may clog small blood vessels in the kidneys. blood clots: COVID-19 can increase the risk of blood clots.High inflammation in the body may cause damage to kidney tissue. immune activity: Some people with COVID-19 have high levels of cytokines, pro-inflammatory proteins made by the immune system in response to infection.Because of this, it’s possible that the virus could be directly infecting and killing these cells. direct infection: Some cells in the kidneys express the receptor protein, ACE2, that SARS-CoV-2 needs to enter a host cell.It’s possible that one or a combination of the mechanisms below are at play: Researchers are still trying to determine how exactly SARS-CoV-2, the virus that causes COVID-19, damages the kidneys. Another 2021 study of people hospitalized with COVID-19 found that AKI was associated with a significantly higher risk of death. 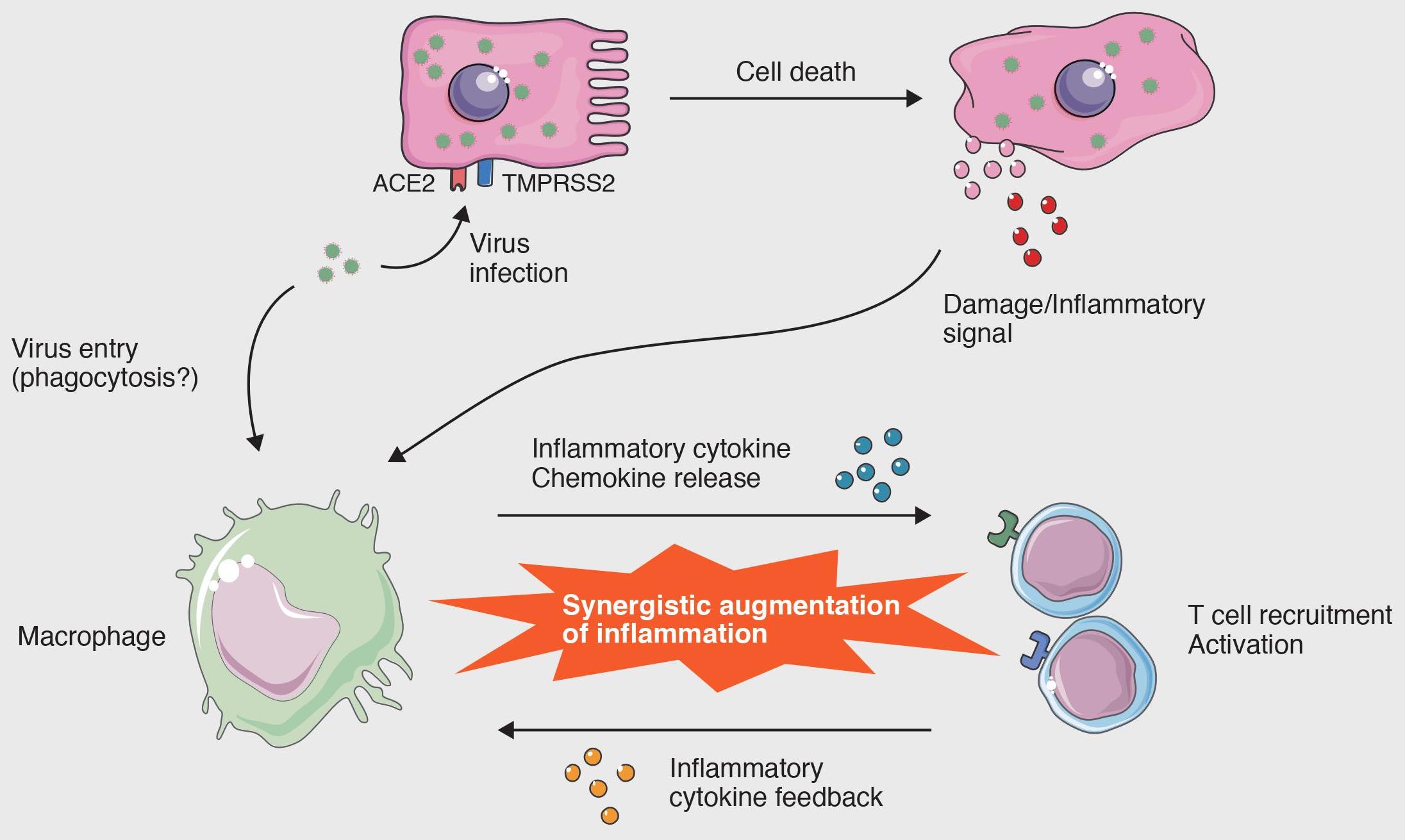
Of these individuals, 347 (19 percent) required treatment with dialysis.ĭeveloping AKI when you have COVID-19 is associated with a poorer outcome. Dialysis helps to remove waste products and extra fluids from your blood when your kidneys have stopped working properly.Ī 2021 study reported 1,835 people with AKI due to COVID-19. 
When symptoms of AKI are present, they can include:ĪKI is serious and needs to be treated in a hospital with supportive care and, in some cases, dialysis. In this case, tests typically pick up on increased levels of protein, blood, or both in the urine. 
In some situations, AKI causes no symptoms and is only detected during testing for other health conditions. This is when your kidneys suddenly stop working as they should. However, the causality needs further identification.ĬOVID-19 VAERS database acute kidney injury vaccination.Many of the reports of kidney involvement in COVID-19 are of acute kidney injury (AKI). 008).ĪKI could occur after the COVID-19 vaccines, predominantly in elderly patients. The proportion of patients on dialysis was higher in JANSSEN than in Pfizer-BNT and MODERNA (14.61% vs. Patients in Pfizer-BNT had the worst outcome with 19.78% deaths, following 17.78% in MODERNA and 12.36% in JANSSEN ( p =. The leading cause of post-vaccine AKI was volume depletion (40.78%), followed by sepsis (11.74%). Comorbidities were noticed in 58.83% of the cases and active infections in over 20% of cases. Most patients are elderly, with the highest age in MODERNA (68.41 years) and lowest in JANSSEN (59.75 years). We observed the differences in ages, comorbidities, current illnesses, post-vaccine AKI causes, and time to AKI onset (all p<.05) among three vaccines. Pfizer-BNT appeared to have a stronger AKI correlation than MODERNA and JANSSEN, based on the highest reporting odds ratio (ROR = 2.15, 95% confidence interval = 1.97, 2.36). The Bayesian and nonproportional analyses explored the correlations between COVID-19 vaccines and AKI. We aimed to investigate the occurrence of post-vaccine AKI reported to the Vaccine Adverse Event Reporting System (VAERS).Īfter data mapping from December 2020 to June 2021, we summarized demographic and clinical features and outcomes of reported cases from three vaccines (Pfizer-BNT, MODERNA, and JANSSEN). Acute kidney injury (AKI), a rare adverse event, cannot be ignored as millions of doses of coronavirus disease 2019 (COVID-19) vaccinations. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
